Case:1
50 year man, he presented with the complaints of
Frequently walking into objects along with frequent falls since 1.5 years
Drooping of eyelids since 1.5 years
Involuntary movements of hands since 1.5 years
Talking to self since 1.5 years
More here:
Case presentation links:
a). What is the problem representation of this patient and what is the anatomical localization for his current problem based on the clinical findings?
Problem presentation:
A 50 year old male diabetic farmer by occupation who had an episode of seizure 10 yrs back presented with c/o frequently walking into objects along with frequent falls,Drooping of eyelids,Involuntary movements of hands & Talking to self since 1.5 years was diagnosed with progressive supranuclear palsy.
Anatomical localization:
Brain
B/l ptosis : weakness of levator palbebral superioris
(without loss of frowning)
self talk : frontal lobe
vertical gaze palsy:
The centres and pathway for vertical gaze palsy is:
supranuclear / nuclear / infranuclear (eg.nmj disorders)
Intact doll's eye, suggests a supranuclear lesion
b) What is the etiology of the current problem and how would you as a member of the treating team arrive at a diagnosis? Please chart out the sequence of events timeline between the manifestations of each of his problems and current outcomes.
Etiology:
Progressive supranuclear palsy: etiology is likely due to accumulation of 'tau' protein in brain
Sequence of events:
Seizures (10 years)
!
T2DM (2 years)
!
Sudden blurring of vision while riding bike -- RTA -- #left leg -- operated (2 years)
!
Frequently walking into objects along with frequent falls
Drooping of eyelids
Involuntary movements of hands
Talking to self (1.5 years)
!
Stopped alcohol & tobacco consumption (1 year)
!
Non productive cough (8 months)
!
Non healing ulcer @ surgical site & hypokalemic periodic paralysis (7 months)
!
Hospital stay for 1 week - diagnosed as PSP & discharged with SYNDOPA 110 MG & QUETIAPINE
!
5 days later patient presented to casualty in a state of unresponsiveness GCS: 3/15 with h/o 2-3 episodes vomiting.
!
Another 2 episodes of generalized tonic seizures happened in casualty - symptomatic management given
!
Suddenly his saturations & heart rate went down with no peripheral pulsations and patient was intubated - CPR done according to 2015 AHA guidelines and was resuscitated.
!
Currently on mechanical ventilator ACMV
c) What is the efficacy of each of the drugs listed in his current treatment plan
Quetiapine:
Quetiapine in the treatment of psychosis in Parkinson’s disease
https://pubmed.ncbi.nlm.nih.gov/17159457/
Syndopa:
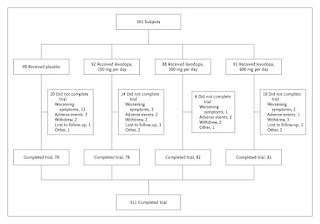
https://www.nejm.org/doi/full/10.1056/nejmoa033447
The severity of parkinsonism increased more in the placebo group than in all the groups receiving levodopa: the mean difference between the total score on the parkinson's Disease Rating Scale (UPDRS) at baseline and at 42 weeks was 7.8 units in the placebo group, 1.9 units in the group receiving levodopa at a dose of 150 mg daily, 1.9 in those receiving 300 mg daily, and –1.4 in those receiving 600 mg daily (P<0.001
https://clinicaltrials.gov/ct2/show/NCT03761030
Case:2
Patient was apparently asymptomatic 2 years back then he developed weakness in the right upper and lower limb, loss of speech.
More here:
Case presentation links:
a). What is the problem representation of this patient and what is the anatomical localization for his current problem based on the clinical findings?
Problem presentation:
60 year old male non diabetic & non hypertensive who had a history of CVA 2 years back now presented with c/o SOB,pedal edema,decreased urine output & generalized weakness since 2 months.
Anatomical localization:
Heart - HFrEF secondary to CAD
b) What is the etiology of the current problem and how would you as a member of the treating team arrive at a diagnosis? Please chart out the sequence of events timeline between the manifestations of each of his problems and current outcomes.
Etiology:
Coronary artery disease (?Cardio cerebral infarction)
Ecg showing:
1)normal axis
2)pathological Q waves from v1 to v6
3)poor R wave progression
suggest a CAD probably involving LAD and LCX territory
Sequence of events:
CVA (2 years)
!
SOB, pedal edema, decreased urine output & generalized weakness (2 months)
!
Started on triple therapy
!
Outcome: Symptomatically improved and discharged
c) What is the efficacy of each of the drugs listed in his current treatment plan

Salt and fluid restriction
https://pubmed.ncbi.nlm.nih.gov/23787719/#:~:text=Conclusion%3A%20Individualized%20salt%20and%20fluid,Quality%20of%20life%3B%20Salt%20restriction.
Ninety-seven stable patients in NYHA class II-IV, on optimal medication, with previous signs of fluid retention, treated with either >40 mg (NYHA III-IV) or >80 mg (NYHA II-IV) of furosemide daily were randomized to either individualized salt and fluid restriction or information given by the nurse-led heart failure clinics, e.g. be aware not to drink too much and use salt with caution, and followed for 12 weeks. Fluid was restricted to 1.5 L and salt to 5 g daily, and individualized dietary advice and support was given.
Results After 12 weeks, significantly more patients in the intervention than in the control group improved on the composite endpoint (51% vs. 16%; P < 0.001), mostly owing to improved NYHA class and leg oedema. No negative effects were seen on thirst, appetite, or QoL
Benfomet as thiamine replacement in alcoholic patients
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4550087/
Aldactone(spironolactone)
https://www.aafp.org/afp/2001/1015/p1393.html
Based on earlier work suggesting a benefit of therapy,2 the Randomized Aldactone Evaluation Study (RALES) was undertaken to evaluate the role of spironolactone when used in addition to standard therapy for CHF.
Case:3
52 year old male , shopkeeper by profession complains of SOB, cough ,decrease sleep and appetite since 10 days and developed severe hyponatremia soon after admission.
Morehere:
Case presentation video:
a) What is the problem representation of this patient and what is the anatomical localization for his current problem based on the clinical findings?
Problem presentation:
A 52 year old male shopkeeper known diabetic & hypertensive presented with c/o SOB,cough,decreased sleep&appetite diagnosed with dimorphic anemia & dyselectrolytemia
Anatomical localization:
Anemia - Bone marrow
Hyponatremia - ? SIADH (lung pathology)
b) What is the etiology of the current problem and how would you as a member of the treating team arrive at a diagnosis? Please chart out the sequence of events timeline between the manifestations of each of his problems and current outcomes.
Etiology:
Dimorphic anemia secondary to ? Nutritional
Hyponatremia secondary to free fluid (dilutional) - poor sugar control (hyperglycemia)
I would rather give lasix and avoid giving fluids as he is having heart failure and hyponatremia which further aggrevates by giving free fluid.
Sequence of events:
T2DM & HTN
!
SOB
Cough
Decreased sleep and appetite (1 year)
!
SOB
Cough
Decreased sleep and appetite (10 days)
!
Admitted
!
Dyselectrolytemia
!
Treated conservatively & discharged
c) What is the efficacy of each of the drugs listed in his current treatment plan especially for his hyponatremia? What is the efficacy of Vaptans over placebo? Can one give both 3% sodium as well as vaptan to the same patient?
No role in giving monocef & metrogyl
Vaptans:
a) Reference
b) Typology of study | a) Vaptan
b) Population
c) Number of patients | a) Interventation
b) Time
c) Main Outcome | Results | Observations |
|---|
Gheorghiade M (Circulation 2003). (26) double-blind, multicentric, RCCT.
| Tolvaptan Hyponatremia in chronic HF. n=254 patients:
| fixed doses of 30, 45, 60 mg/die without fluidic restriction and with stable furosemide doses. 25 days. Primary efficacy variable: change in body weight at day 1 vs baseline.
| A decrease in body weight and an increase in urine output doses-related (p<0.001 for all treated vs placebo).
Decrease in edema and normalization of s[Na+] in the tolvaptan group but not in the placebo group.
Not significant changes in HR, AP, s[K+], renal function. | -A significant number of patients had only mild CHF and modest volume overload. -Necessity of further studies with NYHA-status stratification. -Focused only on diuretic properties of tolvaptan witout mentioning neurohormonal effects.
|
4) Please mention your individual learning experiences from this month.
- A case of ? Broncho-alveolar carcinoma--Lung biopsy - turned out to be organizing pneumonia
- A case of Celiac disease--response to gluten free diet with superimposed giardiasis
- A case of Budd chiari syndrome
- A case of primary PAH
- Cardio cerebral infarction
- A case of ASD (?ostium secundum)
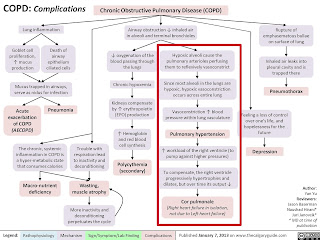
- A case of severe PAH secondary to PTB--lung fibrosis--cor pulmonale
- A case of VSD closure which again become defective
- Rapidly filling ascites
- Renal transplant prospects



Comments
Post a Comment